
The silent killer can no longer hide in the shadows. Wearable tech and the power of medical-grade data can now give us the tools to fight back against hypertension and take charge of our health. In this episode, Dr. Jay Shah, chief medical officer of Aktiia Global, delves into the world of hypertension, wearable tech, and digital health. Blood pressure is often referred to as the silent killer, as it can cause severe damage to the body without showing any symptoms. Dr. Jay explores the basics of blood pressure, why hypertension care is crucial, and the problem of hypertension that millions of people worldwide are facing. He discusses how medical-grade data can now be used to develop personalized care plans. He also discusses the importance of data security, the power of human connection, the impact of artificial intelligence, and more. Tune in now and discover how to control your personal health information to live your best life.
—
Listen to the podcast here
The Silent Killer: Understanding Hypertension, Wearable Tech And Digital Health With Dr. Jay Shah
One thing I’ve been talking a lot about on the show is my desire to understand my body and how that impacts my mind and how my mind, my brain health is impacting the way that I feel emotionally. I’ve shared a little bit about my experience with wearable technology. I have been using an Apple Watch for years, very casually though. I enjoy the way it interacts with all my other Apple products, to be honest. I saw the limitations that it had with sleep. A huge issue in my life is figuring out some of my sleep disorder behaviors and trying to narrow them down.
I then got another piece of wearable technology to help monitor that, and it’s been such an interesting journey because every day I wake up and I’m curious about the data, but then it’s like, “What do you do with this data? Is the data even helpful in figuring out something? Are there going to be answers there?” Our guest in this episode isn’t a sleep specialist but this man, Jay, has a startup based around wearable technology called Aktiia. It’s a Swiss startup but you are not Swiss.
No. I grew up in St. Louis.
How did you get involved with a Swiss startup based around wearable technology? What exactly is the technology? I’ll have you reveal that.
I’ll start with what exactly is the technology. Aktiia is a Swiss company, and the founders over the last decades have developed a wearable technology that can continuously monitor blood pressure in an easy automated and passive way that doesn’t require a cuff or the typical things that we think about measuring blood pressure. It’s an optical sensor at the wrist on a bracelet. That’s the company.
Getting to your point about data is that in blood pressure measurements and hypertension management, as a cardiologist, I was consistently doing this and finding that there were tremendous gaps in understanding someone’s blood pressure, even though we understand and have understood for years that blood pressure is important, hypertension is important, and the world’s most common chronic disease. It’s the primary input to cardiovascular disease and death, but we’re bad at treating it. Only 20% of people in the world who have high blood pressure have it under control and 26% of people in the US.

Hypertension: Only 20% of people who have high pressure have it under control.
A lot of that has to do with a lack of understanding of the data. There are many aspects to it but part of it is people don’t generally put on that cuff and take their blood pressure measurements on a routine basis multiple times a day. What the company is aiming to do is to use the technology, which is this transformative technology but gather and collect a tremendous data set. That’s what we’ve been working on.
Coming back to your first question, how did I get involved in it? It’s a long journey. I’m happy to talk or anything that you want to about it, but I was a practicing cardiologist for over ten years. After a time or over a decade of practice, I wanted to take that expertise and knowledge of real-world practice and then have a different type of impact, have a broader impact on many more people rather than one person at one time. It started me on a journey of exploration and discovery and the result is joining this company at Aktiia as the Chief Medical Officer.
I’m curious about the difference between when you were practicing medicine and caring for clients or working on people’s health conditions versus looking at that data. One difference it seems like that is evolving in the health space is the difference between going to the doctor and having the doctor look at all your health metrics and you as the patient, at least in my experience, it’s been turning everything over to the doctor and letting the doctor be worried about.
The main metric that I’ve paid attention to in my life has been weight. It’s very commonplace for people to have a scale at home. They step on the scale and might see what their number is but other than that, maybe it’s a privilege thing too. I haven’t had a lot of major health conditions aside from my sleep disorder where I have even had to be concerned. For instance, I’ve never paid attention to blood pressure. That in itself is likely a privilege based on the state of my body.
When I see those numbers noted by a doctor, I’m ignoring them. I don’t even think about the numbers again until my next doctor’s visit. For your experience as a doctor, if there is a big transition happening between that type of experience that patients have versus now that they can wear a device and know what those numbers are every day or perhaps multiple times a day and take more agency over it, is that the shift that’s happening with wearable technology?
It’s the shift that people talk about. It’s what we imagine. It’s what we ideate and talk about at conferences. It’s where people say the future is. It remains to be seen how that interface between tech companies, digital health companies, wearable companies and true healthcare delivery. How that integration happens is far messier and more difficult than people might imagine. However, that is the promise of technologies like wearables.
To put it in a broader context, for thousands of years, people would go to healthcare providers of any type. You would have to go to the healthcare location or provider. You’d have to submit yourself through their usual procedures. Everything was built around their process, the healthcare system itself. They then would deliver back a prescriptive response like what you were saying. It’s like, “Here’s the response, Whitney. Here’s what you should do. Here’s the test that we need to run. Here’s the medicine to take. Here are the interventions to try.” You take that, go home, and go on your way until 1 year later, 6 months later or whenever the next time you interact with that group.
In the last twenty years, between about 2000 and 2020, this concept of patient-centered healthcare has come up. People have generally heard about that term but even that, it was still within the context and the walls of a healthcare system. The difference was the patient would be at the center of those discussions, and multiple parts of the complex medical system would be talking with each other about what to do with that patient.
Still, the answer would be relatively prescriptive and say, “Here’s the approach that we think as a collective healthcare system is best for your condition or disease.” Where we’re going in the future or where we have to go because there is no alternative, is what I call patient-driven healthcare. That is where the combination of technology is widely available to millions and billions of people and can enable that step.

Hypertension: Where we have to go is towards patient-driven health care.
What technology does or has the promise to do is not measure things and give you numbers. It’s to give you access to knowledge that before the last several years, people wouldn’t have access to. People who were not healthcare experts didn’t have access to that expert knowledge. You had to go to the healthcare system to access that knowledge. As a doctorate, that’s why people come to see me. It’s not to get a test, surgery or some treatment. They come seeking knowledge, the answer, an understanding of themselves, their health or whatever is going on with them.
In most developed countries, that’s reasonably accessible, although even in the US, there are great disparities and access to that care and knowledge. Beyond developed countries and the rest of the world, there’s very little to no access to that expert knowledge. The real promise and transformational purpose of technology is the dissemination of that expert knowledge. It puts that ability for whatever the condition might be or the aspect might be to get that knowledge on your wrist, phone or through whatever next iteration of technology exists. That’s how I look at the promise of technology in healthcare.

Hypertension: The real promise and transformational purpose of technology is the dissemination of expert knowledge.
I appreciate that perspective, and it does feel quite messy, especially for me who’s in the patient’s position. I’ve been on this journey to figure out what’s going on with my sleep for the past years very heavily. One thing I’ve faced a lot is perhaps what I would perceive as some ignorance or situations in which I’m wondering, “Why doesn’t the doctor have the answers?” I’ll walk away from a doctor’s visit where sometimes I’ve been told, “We don’t know what’s going on,” end of the sentence.
I’m sitting here as the patient goes, “Something’s going on and this is a concern. I’m not going to take, ‘I don’t know,’ for an answer.” That pushed me towards wearable technology because I wanted to be able to collect the data, bring it back to them and say, “Now that I have the data, can you help me?” However, it’s not that simple.
I’ve also done something which I imagine a lot of people do because of technology, which is my research but that’s also very messy because we have so many different sources telling us all different types of information. We know the classic WebMD-type of experience that goes on between patients and healthcare providers, where patients are trying to diagnose themselves. I imagine as a doctor, there must be some frustration there because you can get a misdiagnosis online. How do we work our way through all this messiness to get the real answers that we’re seeking?
It’s not that I have all the answers, but what I would say is that healthcare is almost always going to be messy. It’s not going to be perfect. It’s not a science. That’s why it’s called the art of medicine. Whatever data exists, whatever tests you do and whatever ChatGPT, Google, or whatever WebMD tell you, at the end of the day, the patient is trying to do one thing when they’re sitting in with the physician. They’re trying to tell the physician what’s wrong.
William Osler is considered the Father of Modern Medicine. He was an English physician long ago and he wrote the principle textbook of how to take the history and the physical that’s still taught in all medical schools throughout the country. One of his primary tenets that is still passed down is, “Listen to the patient. They’re trying to tell you what’s going on and what’s wrong.”
Despite all the data, the technology, and the stuff that’s there, that’s coming and that will be there in the future, listening to the person and taking that history in my many years of being a physician is by far the most important thing I can do for that person. Usually, within five minutes, if I’m listening to them, I know what’s wrong. I know what to do and what the next steps are. That’s not because I’m a crazy doctor and a brilliant person. It’s because I have enough experience to know after treating thousands and thousands of patients that there are certain parts of the history that you pick up the data and the knowledge, put it all together and synthesize.
In the future, will ChatGPT do that for me? I have no idea. It might. Who knows? For the time being, the foreseeable future and the existing readers, that’s what we’re trying to do. Data’s important. Wearable data are helpful. Medical test data’s helpful. It’s all helpful but in the end, you’re collecting different parts of history and trying to put it all together. That’s the crux of finding those answers. Sometimes, we still don’t know and that’s the truth. We do have to accept that sometimes.
A lot of times, patients come to healthcare systems expecting them to figure it out for them. Ninety-plus percent of the time, they probably can. A small percentage of the time, they cannot. They will not. They won’t figure it out. They might go to 2, 3 or 4 doctors and maybe the 4th one figures it out or nobody figures it out but irrespective of which type of person that is, it is empowering people to collect their data, have their evidence, show and do their studies at home. “If I did this, this is what happened with my data.” Also, being able to iterate on that and then bring that empirical information to physicians as partners to then, “Let’s sit together and try to piece it together.” That’s what you have to do.
Getting back to this wearable idea, it is the clinical-grade wearable that’s able to do some of those things to create those feedback loops, activation, empowerment and knowledge. That’s what matters. A lot of the other features and wearables are fluff, honestly. It’s like, “We’re trying to sell devices. Let’s put in some random stuff and people will buy stuff.” However, when you’re trying to create something of value for a patient, you have to figure out how to empower them and make them understand things more.
I imagine it’s going to take some time on three ends, perhaps. We have the companies like yours where you, as a team, are committed to creating something valuable and not just fluff. That’s a big responsibility because, in a capitalist society, companies are saying, “Wearable technology is cool and trendy. People are willing to spend their money on it.” Maybe we give somebody peace of mind because they’re wearing something on their wrist.
The downside is it can be very confusing. I’ve certainly found with this new wearable technology I have that it didn’t make a lot of sense to me and still has a way to go. It’s giving me enough where I feel satisfied but it’s very confusing and messy. There’s the side of technology that has a lot to work through. There’s also the customer or patient education itself. “What data is important for me to know? What should I be paying attention to? How do I conduct my experiments?”
However, there’s also the practitioner side, the doctor or physician side of it. My experience is I’m a little ahead of the game than the physicians I’ve worked with. I walk in there and say, “I have a wearable device. It’s telling me these things.” Most physicians stare at me blankly. They don’t know what to do with that data. I feel like, “What do I do? How can we create that partnership?” What do you see evolving in all three parts? Do we all have to work together to make this happen? How long is that going to take?
It is going to take a long time but the truth is it is more than three also. First of all, let’s start with the physician’s skepticism, lack of understanding and unwillingness to take it. You have to remember it. In the current model of healthcare, physicians are going to use the data that they trust. There are a lot of reasons to not use any data that isn’t trustworthy. Scientific methodologies can be skeptical until the data is proven to be accurate and reasonable.
For example, wearables can create all kinds of data sets but have they been validated? Have they been tested rigorously and scientifically? Are they regulated by regulatory agencies? It’s because that’s a high bar to pass scientifically to then be able to be a regulated medical device, which most wearables aren’t and don’t have any components of.
Physicians are not used to taking data from this unregulated sphere of products. When we order tests, they’re all regulated devices. They all have had to pass pretty rigorous specifications to be able to say, “We can use that data for clinical decision-making.” Generally, physicians are going to be less willing to take unregulated data and say, “I’m going to use that to make decisions on this person.”
At this point, we’re in the infancy of this wearable health tech space. There’s still a lot of fluff. There’s a lot of data that isn’t validated. There are categories of devices or features of devices that are unregulated. How much can you rely on that data when it comes to medical decision-making? That’s where physicians are generally coming from. There has to be more testing. The companies, the physicians and the healthcare organizations have to do more evidence-based research using those devices and gain that trust and that takes time, money and effort.
What generally happens is that consumer-grade companies or consumer electronics companies have never played in that space of regulated medical devices. It’s a very different model than selling directly to consumers with like, “You can get your text messages on this thing.” That’s unregulated and honestly, not that difficult from a medical evidence standpoint. They have to consciously make a shift to say, “We’re going to put a huge amount of resources. If we want to be trusted by healthcare, then we have to prove that we are trustworthy.”
There’s a big gap between wearable devices and trustworthy medical devices. There are very few companies that have traversed that gap to say, “We are going to go down that giant rabbit hole, take that effort to become a regulated medical device and show our quality and standards.” There’s so much in this unregulated space so it muddies the water and creates a lot of noise.
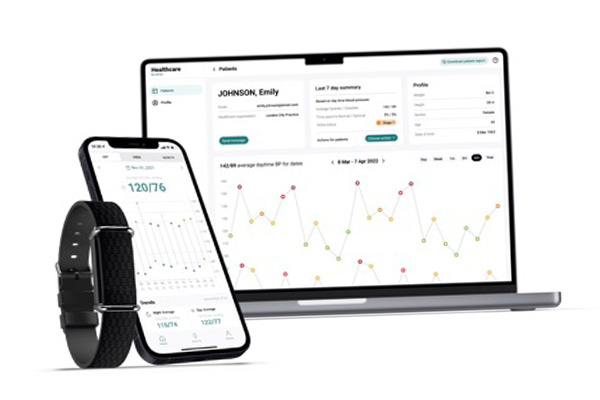
Hypertension: There’s a big gap between wearable devices and trusted medical devices.
For example, in our companies, we are a regulated medical device. We’ve done that. Some others have but there’s so much noise coming from this other side that it’s hard to pick out for most physicians and even people. It’s hard to pick out which one is trustworthy, which one has evidence or which one has scientific data behind it if I’m going to try to use it for health. That’s a very muddy pool. Those things will consolidate.
Regulatory agencies are already starting to write some guidelines to say, “Here’s what we would consider. Here’s what you need to do to clear these thresholds.” In healthcare, it is a very slow process. We will start gaining evidence from certain devices with companies that try to get that evidence spelled out and then they’ll have more answers.
When you do bring that one specific device that they understand and have seen that they can trust, they’ll say, “I can use that.” Unfortunately, it takes a long time to get anything innovative changed in healthcare because there are all these different aspects to it. Generally speaking, from innovation to being in the healthcare market takes roughly seventeen years.
Where are we in that timeline, if you were to guess?
For each innovation, if you develop some new device, product or thing, generally, it takes seventeen years and that’s on average. It’s a long time for each one of these things. You then pair that with a capitalist market. Many of them are venture-backed companies, which means that they have to show a return within 3 to 5 years. There’s going to be a lot of them that don’t work out and that’s the nature of it.
It’s probably for the better. The other challenge with the case of new technology is the expense. The Apple Watch is not that cheap. It’s something I’ve justified over years of having one. To your point, I don’t view the Apple Watch as a medical device. They’ve developed some elements over time but that’s not why I use them.
When I got the newer piece of technology, I wanted more data about sleep but I have to take some of that with a grain of salt given I don’t even know. You’ve inspired me to go check and see, “Is it regulated?” You know what device I have but I won’t mention it. I don’t know that much data and that’s something interesting as a consumer too, not understanding what might be important.
A lot of these tech companies have the money to spend on marketing. They can be very savvy about it. They are probably thinking the consumer doesn’t either need to or want to know some of this information. They’re only looking for a quick fix or something more superficial. Also, there’s all the hype involved. When I started considering wearable tech beyond the Apple Watch, I was very skeptical. I’m a huge Apple products enthusiast. Maybe at this point, I have everything they make. I love it.
It is not that hard to influence me but I still felt skeptical. I’m like, “I don’t need a watch.” I’ve never been a big watch wearer. It wasn’t until I was gifted one that I got excited about it and then it’s like, “I can’t see myself not wearing it.” With the other wearable technology, I’m in the newer phase of skepticism and thinking, “This could be a short-term thing for me. I’m not sure about this.”
The one that I have is a subscription model. I feel a little uncomfortable about that. I don’t know how Aktiia works in terms of your price model. I would love to hear your thoughts on it. The subscription model makes sense because it gives me flexibility. I can try out the device and if I don’t like it, I’m not attached to it. I don’t have to spend any more money on it.
However, if I do want to stick around with that, it makes me a bit uncomfortable too. The annual fee of this device that I’m using is around the cost of the flat fee of the Apple Watch. My Apple Watch I’m finding works well for many years since buying it. The cost of this wearable technology can be high over many years. Is that beneficial to the consumer and the patient or is that getting in the way of people utilizing this technology?
I don’t know that I have the answers for all of it but from our standpoint in Aktiia, we sell on a flat one-time purchase. One of the downsides that I’ve learned as I’ve been in this role of selling anything that involves hardware is that it’s extremely difficult to make a profit if you have to manufacture hardware. These larger companies like Apple, Samsung and the giants of consumer electronics have figured out the manufacturing. They’ve built factories themselves. They’ve gotten the cost down as much as they can. They charge a premium fee.

Hypertension: One of the downsides in selling anything that involves hardware is that it’s extremely difficult to actually make a profit.
For a lot of them, you’re in their ecosystem. Even though you’re not paying a subscription for that device, you’re paying in other ways and we all do that in some part of the subscription model. That gets you with that ecosystem. The challenge with one-off wearables, a separate thing that exists as proprietary hardware is what you said. It’s very difficult to create a payment structure that would create sustainability for the company. Otherwise, they’re not going to make money and they’ll not be around. That’s one aspect of it.
Subscription models make sense if they provide significant value. What is that value, is the question. How much value do they provide? It depends on the company. That’s the point. If we’re thinking about a subscription model, let’s say in Aktiia, we have to think very carefully, “We’re a regulated medical device. Hopefully, people will recognize how difficult that is to achieve and how much resources it takes to do that.”
Number two, you have to show that you are able to do something that provides either data or an interactive experience that is so significantly valuable to that person that they’re willing to pay a few dollars each month or whatever it is that the company is charging. We’re working on it but that’s a big challenge. One of the things about Aktiia is that overall in the long-term, we have architected the system so that none of our hardware is proprietary. It’s all in the software.
In the long-term, with some partnerships, we hope to be able to ride on top of other wearable devices as software so then you don’t have to manufacture the hardware. You don’t have to wear two pieces of wearables or more. It allows you to expand your install base and your reach in terms of access to people. However, that’s hard to do unless you’ve built it from the ground up without proprietary hardware. That’s a challenge because many wearable companies have done it with proprietary hardware.
In that scenario, that’s a difficult thing to sell because you’re realistically never going to compete with those giant consumer electronic companies. Either you’re going after a very niche market where you are like, “I’m going to go after this one small slice and get good at that,” or you’re going to get acquired or not going to go anywhere.
This is all fascinating to me. I’m interested in the monetization structure. That transparency is beneficial to the consumer. One reaction I had listening to you talk about that is compassion. I’ve been sitting here going, “This company is trying to extract all this money from me. I feel a little bit resentful or annoyed that I’ll have to renew if I want to stick with this thing.” However, compassion comes up like, “If I know that my money’s going somewhere that can keep the company afloat so I can continue using it but also, if it’s going toward the development of a product that is helpful to me in the long run, I’m more likely to keep my money there.”
Perhaps you could say the same thing with Apple. I’ve been a very long-term user and I believe in them. They’ve earned my trust. They’ve never let me down. I have a good relationship and it’s easier for me to say yes to spending my money. It’s a premium product. Even these headphones, for example, they’re insanely expensive in the market compared to the competitors but Apple’s overwhelming influence on me helped me justify spending more money on something that I probably could have saved and bought something else.
As a consumer, some of this psychology is helpful and I appreciate your transparency. That leads me to another resistance point that I’ve heard. My dad is a great example. For the holidays in 2022, my sister who convinced me to get the device I have, wanted to buy the same one for my mom and dad for their holiday present. She’s thinking, “This data is going to be so helpful for their health. They’re going to love it.” She gave it to my mom. My mom gets it. She barely knows how to use the app because this device requires you to use your phone. There’s no screen on the device I have. My mom needed a lot of education but she still wore it.
My dad was very concerned about data privacy and this comes up a lot for people that are thinking through this. I’m someone who loves data and I’m willing to give away some of my privacy to acquire data for myself. I’m willing to give away some of my data for advancements to happen if there’s transparency in how my data is being used. My father, on the other hand, is very skeptical and concerned about data privacy. He is not willing to take a lot of risks, thus he returned his wearable device because he was too afraid to use it. Can you speak to any of the data privacy sides of it for people that are concerned?
It’s one of the problems of our time, honestly. We see that in all respects, not just in wearables but in all the accounts. We have internet accounts, search accounts and social media platforms. We’re seeing it all over the place. If you’re online at all, which is almost all of us in most of the developed world, it’s very hard to know who has your data. You don’t know. I don’t know. I don’t think anyone knows who has my data or pieces of my data out there. That’s one aspect that I’m certainly not an expert in but that is a major concern for us. Some people are less concerned about it than others.
If you're online at all, which is almost all of us in most of the world, it's very hard to know who has your data. Share on XThe next generation hopefully, will be more concerned about it because a primary monetization strategy of a lot of these companies is selling your data. We’ve seen that in a number of ways. That’s the more cultural and social aspect but on the medical side, on the healthcare side, there’s a very significant concern for what’s called Personal Health Information or PHI.
If you have a medical product that is in the world and is collecting data from you but then that data is going through a cloud server to somewhere else and that data are flying around, there has to be fairly strict end-to-end encryption. There have to be server protections and cybersecurity threat risks plans and all these different things in place that a lot of them are regulatory-driven. There’s a huge push from regulatory agencies to focus on data security and data privacy.
In the end, none of it is bulletproof. How many times have we seen some companies pay millions and millions of dollars for security measures and then they get hacked? It is bound to happen in a digital world. That is somewhat of a trade-off but as much as we can and as much protection as there can be, we have to have that end-to-end encryption in the data privacy and cybersecurity rules.
Any company that even wants to think about healthcare as a significant part of its product is going to be held to those very high standards. That’s another area where all of these things, anytime there’s a regulation, risk, security and privacy involved, it adds to the complexity in the cost of delivering the product to us in the consumer’s hands but it is a huge concern. It’s already forefront in the minds of regulatory agencies. I don’t think it’s going to continue to be pushed as a primary need from any type of wearable or any company that’s delivering data to multiple sources.
The other thing that seems to come up along the same lines is ChatGPT. I am very interested in artificial intelligence but trying to be a little bit more skeptical. It’s easy for me to get excited about developments that save me time. Artificial intelligence is a tool that I feel like I’m using in conjunction with my brain, much like I see a wearable device as a tool that’s giving me information that I can then do something with.
However, there are people concerned that wearing these devices is making us cyborgs. There are fears of the advancements in technology and how that might interfere with the human experience. I’m curious about your thoughts about that too. Are we headed in the direction where we’re constantly tethered to technology? What are your viewpoints on where we stand with that and the pros and cons?
I don’t know if you’ve seen Stanley Kubrick’s 2001: A Space Odyssey, but when ChatGPT first came out, I immediately thought of HAL and I was like, “We’re there.” I don’t know, honestly. That’s going to be an overriding concern. With quantum computing and generative AI, we’re at a different inflection point regarding how technology’s going to impact our world going forward. However, at the end of the day, it’ll be a tool. It can be used in a lot of good ways equally well. Also, it can be misused in a lot of ways. As far as I can tell, in my nascent knowledge of this, there’s no clear way to regulate it.
There are risks involved but having said all that, it would be foolish to discount it and say, “No one’s ever going to adopt this.” It’s not true. They are going to adopt it and it’s going to be applied incalculable ways. From my perspective as a physician, you got to get ready for change. Maybe that becomes your assistant or a part of your daily practice somehow in the future.
We have to be ready for change. We have to be ready that maybe AI or technology can become our assistant, a part of our daily practice, and more. Share on XMaybe it helps you speed up in certain ways or slow down in others. Try to look at it optimistically. Try to incorporate it in sensible ways but still for the foreseeable future, unless someone invents a robot with ChatGPT inside them to then become a nurse, which would be very odd or a physician, maybe that’s a little far off. In the end, you can get multiple recommendations from ChatGPT.
You can even get a reasonable diagnosis list from ChatGPT but who’s going to do that? Who’s going to execute the plan? Who’s going to walk you through chemotherapy? Who’s going to sit with you in the hospital? Who’s going to talk to you about how to go to hospice? Who’s going to tell you about, “Here’s what surgery looks like? Here’s what it feels like?” Who’s going to talk to your daughter or a son when you’re unconscious in bed or there are only ones left to talk to?
That’s the human element of medicine that I don’t see AI taking over for at this point. After several years in medicine, to be very honest, that’s the most important part of our job. The knowledge part of getting to the right diagnosis or giving the right medicine is the easier part. It’s the human element that is much more difficult. Maybe there’ll be a time when people stop wanting that or stop caring about it but my guess is as human beings, that’s pretty far off.
That’s so beautifully said and it’s such an important reminder because I see so many technology benefits. I’ve always been drawn to it my whole life. I see it as the tool that we’ve been talking about. I see it as a form of expression. There’s creativity and data involved. I see it as helpful. I also haven’t lost my desire for human connection. I feel confused and people get so concerned. Maybe it’s ignorance. I do feel like the two can work in harmony,
It is that messy time when we’re figuring it out. A lot of this is very new, to your point. This needs a lot of time. Artificial intelligence has been around for a while and yet it feels like it just started based on the rise of tools like ChatGPT, which have only been in the public conversation in this way for 4 or 5 months as of the time of this recording. Yes, it goes way back before that but the adoption curve, we’re still on the upward side of it and have a long way to go. There’s so much that remains to be seen.
Artificial intelligence has been around for a while and yet it feels like it just started. Share on XI’d love to come back around to some of the basics of why you’ve been involved with this company. Why does this product exist? As I said from the beginning, I have a lot of ignorance about blood pressure so I want to make sure that we touch upon this before the end of the episode. Perhaps it’s a privilege to have not yet in my life been concerned with it. I don’t understand hypertension but I’m trying to.
When I went through my well-being coach certification program as of April 2023, I have a long way to go to learn about it. However, as a wellness coach, part of the code of conduct is to understand. My understanding is the metrics. I know what good blood pressure looks like metrics-wise but I don’t understand yet what it means. Could you break that down into terms for anyone else who like me is feeling a bit ignorant?
Let’s do some blood pressure 101. With blood pressure, as probably most people know, you get a top number and a bottom number. The top number is called systolic. The bottom number is called diastolic. The top number reflects the pressure within the major arteries of your body during a heartbeat. When the heart squeezes and pushes all the blood out, the blood has to move down the arterial tree and there’s a distension of the arteries. That’s the peak of the pressure. That pressure is reflected in the top number as systolic blood pressure.
In between heartbeats, the distension of the blood vessels goes back down to normal. The blood gets pushed down to the organs and it gets back to a steady pressure between heartbeats. That number is the bottom number. It is called diastolic blood pressure. Neither one is necessarily much more important than the other. They’re both important. They both reflect different parts of the cardiac cycle and the pressure in the arteries and that’s what blood pressure is.
Hypertension or high blood pressure is a very exceedingly common problem. 1.4 billion people in the world, 130 million people in the US and 1 in 2 Americans over the age of 65 will have high blood pressure or has it. Generally, high blood pressure starts even when someone’s in their 20s, 30s and 40s of life. It’s not necessarily a disease of the elderly. It starts earlier. You don’t feel it. There are no symptoms so people generally don’t know that they have it.
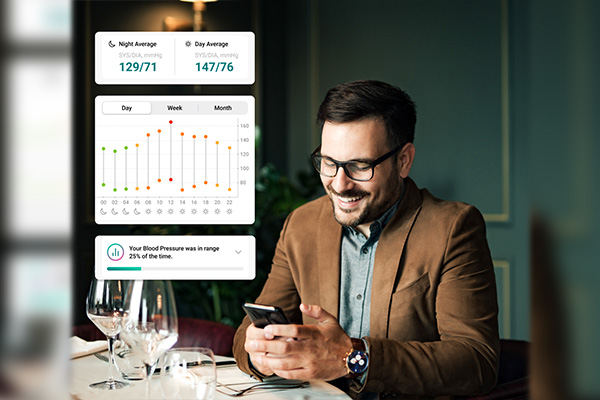
Hypertension: High blood pressure is not necessarily a disease of the elderly. It starts earlier, you don’t feel it. There are no symptoms.
Almost half of the people who have high blood pressure don’t know they have it. What 30-year-old is going and routinely checking their blood pressure on a routine basis? There are not many and nobody goes to the doctor generally very often when you’re young because you don’t have any problems. That’s human nature. That’s what high blood pressure is.

Hypertension: Almost half of the people who have high blood pressure don’t even know they have it.
People understand conceptually that high blood pressure is tied to heart disease but it’s tied to many things. It’s not just heart disease. It’s heart attacks, strokes, kidney problems, kidney failure, arrhythmias, heart failure and reproductive problems. There can be problems after pregnancy and high blood pressure. There can be problems during pregnancy and high blood pressure. It’s tied to diabetes. There are a number of problems. It can cause vision loss.
There are countless other medical problems for which the primary input for those problems is a history of high blood pressure. High blood pressure is a risk. The main downside of having high blood pressure is time dependent. It’s not one day of having high blood pressure. It’s not 1 minute or 1 hour. It’s not even 1 week or 1 month. It’s years of having uncontrolled or less controlled high blood pressure.
It’s years of spending your life in a higher-than-normal range of pressure. Over that time, that higher pressure does damage to the tiny vessels of your brain, eyes, kidneys, heart and everywhere else. That’s how it causes its damage. That’s how it leads to its damage. That’s why it’s called the silent killer because it’s silent. It doesn’t have symptoms but in the end, it causes about 18 to 19 million deaths per year. There are 20,000 deaths a day just from hypertension.
That’s why it’s such a big problem. The way the medical system is designed, it’s designed to be reactive. It’s designed to treat a problem that exists now and help you when you’re having a heart attack, a stroke or a kidney problem. It’s not designed to be preventive or proactive. “Let’s solve the problem ten years before it happens or let’s try.” That’s why hypertension is poorly managed, even though we have lots of treatments for it and a good understanding of the disease. That’s what high blood pressure is and that’s why it’s important.
It’s helpful for me and I appreciate that because we all learn differently. Until I started studying well-being to get my certification, this didn’t make sense. I’m still trying to conceptualize it and put it into practice. Having not been exposed to something can lead to a lot of ignorance. I’m curious about what you believe are the best ways to be proactive given that the medical system isn’t necessarily leaning on or focusing on that. Is that where the device comes in where you know your data and if you’re seeing the data, how much can you do to influence it? How long does it take for the lifestyle changes to make a difference in your blood pressure results?
That’s exactly how Aktiia thinks about it. In between your once-a-year visit with your physician or healthcare team or maybe less than once a year, there’s all this time that goes by. How can we give people accurate, validated and regulated medical grade data and wrap around that data activation plans and care plans? How can we empower them to look at that data to understand what it means and how some part of that is in their control?
They can go out and say, “Here are the five things you can do to try to change what we’re seeing with your data,” and then see what changes. Generally, lifestyle changes for high blood pressure could include salt reduction, exercise, activities, dietary changes and weight loss. There are a lot of sleep disorders connected with high blood pressure. It depends but it generally takes a couple of weeks to start seeing a significant effect. Some of them could be quicker but usually, it’s a few weeks until you see that your change is making a difference.
It’s also sometimes difficult to measure that change when you’re looking at one measurement at one point in time. It’s because blood pressure fluctuates every day, up and down, hour to hour, minute to minute. If you only get one measurement out of this big long curve, how do you know? Are you making a change or not? Is that day just a bad day or did you catch the peak? You have no idea.
That’s where the idea of continuous passive, automated blood pressure measurements gives you that entire trend. It gives you the whole moving picture rather than the snapshot so you can understand, “Here’s my pattern. Here’s the average. Here’s what it looked like before I did Dry January. I did Dry January and then here’s what happened at the end of January. There was no difference. I did that and there was a significant improvement.”
Those are things that are empowering for people. For hypertension, in particular, we don’t feel it. One of the major gaps is that we give people recommendations. Physicians always talk about sodium reduction, exercise and so on. The person might do it for 1 month or 1 week or 2 but they don’t feel any different. They check their blood pressure occasionally and they’re like, “It looks the same. I don’t think it is very working very much.”
There is no feedback loop to encourage them to continue with that positive behavior. We try to build that in as a digital feedback loop to say, “This intervention you’re doing is working. Keep it up,” or, “This intervention’s not working. Don’t spend your energy doing this. Let’s go on to the next three things you can do.” That happens a lot in hypertension. People aren’t one size fits all but our treatments are one size fits all. Hypertension is a great example of that.
If you go to the doctor for hypertension or I go to the doctor for hypertension, we’re going to get almost the same answers about everything like diet, exercise, weight and medications. Everything’s going to be almost verbatim or the same but we’re two different people and our bodies are going to respond in two different ways to any one of those interventions. Here are the things that physicians don’t know what you’re going to respond to. We don’t have data or science on that.
This is another major gap. If we have this granular continuous data set, we can look to see what changes make a difference for you and which intervention made a difference. If you’re starting medication, which medication might work better for you than others? Also, start to get personalized about hypertension care and do it at scale, which is what’s required for hypertension. That’s what we’re trying to do at Aktiia.

Hypertension: If we have this granular continuous data set, we can really look to see what changes make a difference for you.
That is so inspiring to me to hear all of these details. The other thing I’m curious about is the tracking side of it, which I’ve been working on for quite some time. I’ve dabbled in a few different apps and find that hard to understand and track my memory even with the wearable technology that I’m using. Every morning I wake up, it has a journal questionnaire type of thing. I’ll find myself like, “I don’t remember what time I did this or that. I don’t remember exactly how I felt,” even though I have a good memory. It’s still hard to remember all those little moments in our day.
I’ve also tried through other apps, tracking throughout the day but that would get pushed away. I’d get focused on something. Tracking yourself and all the little changes is hard. The other thing I found, even with the tracking, with all that data compiled after months of using some of these apps, the conclusions and the summaries I would get wouldn’t be as conclusive as I would like them to be.
I want someone to say, “The fact that you drank enough water added up or the steps that you took.” You mentioned these things like diet or exercise. Most of us know these things are beneficial but for someone like me who’s very data-oriented, I would like to know, “Does it make a difference if I drink 4 glasses of water versus 8? Does it make a difference what type of exercise I do?” How do we figure out all of that? Is it not that important in your experience to know that finite?
There are a couple of things. First of all, as we think about it and other companies probably think similarly, the more we can get about your activity passively without the user having to go in and annotate something, the better but that’s hard because the sensors are only going to pick up certain things. The accelerometer will pick up motion. You can derive activity from that.
Your optical sensors will give you blood pressure and heart rate. That’s transformative in and of itself but those are just three parameters. What’s crucial is to build that valuable data set of physiologic parameters but then around it, enable the person to start annotating that data set. That takes some active participation and this is where the consumer wearables have in some ways done this part of our ecosystem a disservice because we’re so used to having everything automated.
You click it and it works. You open it and it works. You click on the phone and the Apple signal comes on. It works. Your email’s there and your texts are there. You don’t have to think about it but that doesn’t work when you’re talking about your health and physiology. If you want to know, for example, how much water intake had an impact on your heart rate baseline, the sensor is never going to be able to tell you how much water you’re drinking. The only way for that app to pull in that data is for you to enter it.
There are countless other things that you could think about like medication adherence or what type of exercise. That’s a good one. “Was I walking? Was I biking? Was I running? Was I jogging? What was the exercise? What happened with my physiologic parameters?” It’s generally not going to be able to tell you without you putting in that data yourself.
Your sleep tracking is another pretty difficult one. Yes, you can probably detect with an accelerometer when someone falls asleep and when they wake up but it can’t tell you how many glasses of wine did you have before you went to sleep and did that affect your sleep and all the other things that might be parameters. Getting back to value from the device, if people want to get more value out of the device, they will probably have to have more bidirectional data flow between the user themselves, the device and their interface.
It’s not going to be automated like what we expect with our phones, watches and other things. It’s super automated. It just works and we like that about it. I like it too. Everyone likes it but that has gotten us into a mentality that everything can be that way and that is simply not the case when you’re talking about health data and annotated data sets, it’s not going to have a sensor that does all those things.
Jay, I will say that I do have one thing that gets me close, which is a water bottle that measures how much water I drink throughout the day. Maybe I’m the exception, but that syncs to my Apple Watch, and I have a little thing. It tells me how much water I’ve had but what I don’t know, to your point, the data isn’t coming to a conclusion. Even though I can sync them together, it’s still a bit vague, and that’s probably where the software has some way to go or maybe I’m using the wrong wearable. That’s a question.
They have these health toolkits that will compile data from all these different sources but do they allow the bidirectional flow of that data? Do they allow your data from your water bottle to go to your other wearables app? My guess is that it doesn’t. If that’s the case, you have to say, “What’s the point then? If it goes into this one but doesn’t go over to this one, why not? Why can’t they open those doors?” They can. There’s a reason that they haven’t. It’s all proprietary, this and that. They don’t want to share but if you had a way to compile it and the doors were all open, there was a lot of data shared.
Data sharing, not just in wearables but in the medical healthcare data itself is a big issue because traditionally, they have been siloed data sets. One organization’s data doesn’t talk to another organization’s data when the payers can’t access it. There are all disparate data sets. Some giant huge fields and experts are talking about this. How do we enable data sharing when we have trillions of exabytes of data that could be useful when putting it together but they’re all in different places and platforms? The same thing goes with these wearables.
I imagine I’m an outlier in the average consumer base that doesn’t want to have to deal with all that. Even though I am very interested in it and very tech-skilled, I still feel confused. It still feels messy and frustrating. I still have days where I don’t feel like typing in anything and answering questions. I want to be left alone. I keep coming back to all of this because I want to feel good. I want to feel my best every day. I would like to live a long life with health.
The statistical data you are sharing in this episode is a great reminder of that for me, Jay, and answers some questions. I had one day when I saw multiple doctors and I didn’t understand why my blood pressure readings were different at each visit. I walked in and said, “You don’t need to do my blood pressure. I had it done at the other doctor.” They did it anyways. I was like, “What? Why are they different?” You have my curiosity very piqued. I can’t wait to see, “Do either of my devices measure any of this?” If not, you might have me as a customer because I’m curious and I want to take good care of myself.
You’re not alone in that sentiment. There’s a challenge getting back to this question that you posed before between the human side of things, technology, and how that affects our health and brain health. One of the things that we need to always remember and there are some great examples of this is that there are many determinants of true wellness and happiness if we can use that as a scientific term.

Hypertension: There are many determinants of true wellness and happiness, and it has little to do with scientific data.
If you look at studies that have been done on people trying to understand who has a better sense of their wellness and happiness versus others, it has pretty little to do with scientific data or technological inputs. It has to do with socialization, human connection, and friends and family. That is magnified by a large-scale study that you probably have seen in major press media about the detrimental effects of social media on both young and older people.
We need to always remember that there are many determinants of true wellness and true happiness. It often has little to do with technological inputs and more with socialization or human connection. Share on XIt has tremendous negative mental health side effects, and it’s so clear that there’s an addictive process there that is detrimental, especially to our younger generation. That’s an area that we need to focus on that although we have all these devices and stuff around us, as humans, we still need that human connection. What we’re seeing in the outcomes of these studies is that there’s a lack of that human connection because everyone is on their screen connecting with somebody else. It is not the same as walking down the street and having a conversation, going to a movie or having traditional interactions.
That’s one of the benefits of wearable tech, in my opinion. One of the reasons I’ve enjoyed the Apple Watch for so long is I don’t have to carry my phone with me. The things I was dependent on for so long with my iPhone, I get a lot of those same things on my wrist. Sure, it’s still tech. It can still be distracting but it gives me a better chance of connecting, being present and making eye contact.
To your point too, the other device I’m using does ask me each day how much time I connected with friends and family. I’m grateful it does. The data still is a little inconclusive, but what I wish it would ask me is how much time I spent on social media. That side that Apple added and Android did as well is you can go and see how much screen time you spent. There’s a breakdown.
I’ve been off social media. I would be curious. What were some of these data points before and after? That’s where another benefit of data can come into play for people. As much as going to the doctor and getting their blood pressure read or maybe they’re using a device that does it at home, if people were presented with more data about these determinants of our health, maybe that would help them make decisions versus you read these news stories and they’re often sensationalized. The media does that. They might not apply to you whatsoever.
We go about our days thinking, “Maybe we’re the exception or we’re in a different category.” I’m very passionate about raising that awareness around things like social media. I’m so glad you brought that up, Jay. A beautiful thread through this conversation was the human connection. I hope we’re modeling that in our conversation. To me, this is why I much prefer podcasting to creating social media content because I want to connect with people like yourself.
I want to connect with the people who would spend an hour with us doing a deep dive and thinking things through. I am grateful that you brought up that reminder for us to consider. It’s more than just all the little health metrics that we’ve been taught throughout our life. Also, all those choices and changes but beyond us, there’s so much at play in how we impact one another.
There's so much at play in how we impact one another. Share on XThat gets to how I always at least try to coach and speak to my patients. We want them to live longer and feel well but the purpose of all of that is for them to have happier, more connected, and a sense of well-being in their life. That always is the driving force, at least, for me, in my conversations. Whenever I bring that up with patients, they universally connect with that. That tells me that that is a nearly universal feeling. It’s never like, “I want to live until I’m 93 or something like that.” It’s always like, “I want to live well.” That’s it. That’s what they want but with medicine, we could do a better job usually in talking about that.
Thank you for being a positive role model for other people in your field and also, for other wearable technology. I feel like you’ve raised the bar. You’ve set a high standard and hopefully, that can help cut out some of the fluff that we’ve talked about and help people make better decisions for themselves. Ultimately, the big aim of conversations like this is to have the data and the inspiration so that you can choose what works best for you.
I appreciate the way that you approach that, your transparency, and your awareness of all of these important factors and our well-being. It is beautiful to witness. Thank you so much, Jay. I’ve learned so much from you. You’ve motivated me and sparked my curiosity in ways I wasn’t expecting. I’m grateful for that.
Thank you so much.
For the readers, I will be back in the next episode. Bye for now.
Important Links
- Aktiia
- Hidrate Water Bottle
- https://www.Facebook.com/AktiiaGlobal
- https://www.Instagram.com/AktiiaGlobal/
- https://Twitter.com/AktiiaGlobal
- https://www.YouTube.com/@Aktiia
- https://www.LinkedIn.com/company/Aktiia/
- https://www.LinkedIn.com/in/JShahMD/
About Dr. Jay Shah
 Dr. Jay Shah has 15+ years of medical expertise and 11+ years of leadership in the medical practices at city general hospitals, to community settings, to the Mayo Clinic. He has brought his experience and expertise to the Swiss startup Aktiia, to change the paradigm of how the world’s most common disease – hypertension – is understood and managed. Also an angel investor and advisor, he is passionate about applying technology to solve practical problems in medicine and believes strongly in the power of positive thinking and collaboration.
Dr. Jay Shah has 15+ years of medical expertise and 11+ years of leadership in the medical practices at city general hospitals, to community settings, to the Mayo Clinic. He has brought his experience and expertise to the Swiss startup Aktiia, to change the paradigm of how the world’s most common disease – hypertension – is understood and managed. Also an angel investor and advisor, he is passionate about applying technology to solve practical problems in medicine and believes strongly in the power of positive thinking and collaboration.
Love the show? Subscribe, rate, review, and share!
Join the This Might Get Uncomfortable community today:



